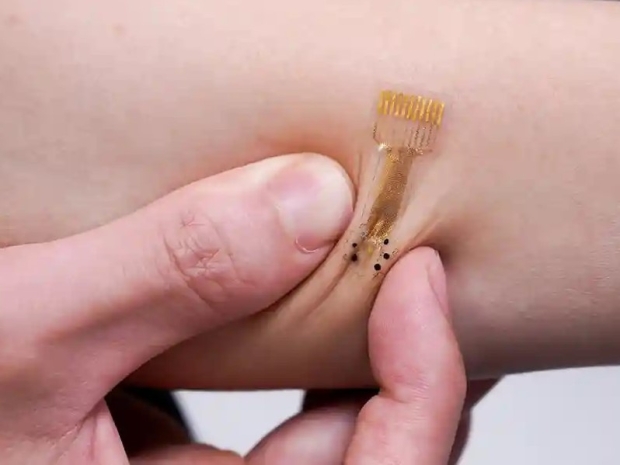
California Institute of Technology’s Dr Wei Gao said the device consists of two parts – one reusable flexible printed circuit board and one disposable patch. The disposable patch contains biosensors, electrodes, and drug-loaded hydrogels.
The biosensors mean the “smart bandage” device can monitor features of the wound such as its temperature, pH, and levels of substances including glucose, uric acid and lactate – metrics that provide important insights into whether the wound is infected and its levels of inflammation.
The device allows for electrical stimulation to be applied – a technique previously found to encourage wounds to heal, but which has been hampered by bulky equipment. It enables the controlled released of anti-inflammatory and antimicrobial drugs.
“All the signals can be wirelessly sent to a user interface [such as] a computer or a mobile. We can wirelessly control the drug release by applying electrical potential.”
According to Science Advances, the team describe how they tested the smart bandages on wounds of diabetic mice and rats before and after infection, finding the devices detected features including the temperature, glucose levels and pH of the wound fluid. These measurements changed as expected before and after the mice were given treatment.
Mice with smart bandages who experienced drug release and electrical stimulation showed higher rates of wound closure and less scarring than mice whose wounds were not covered by the bandages.
The team say they expect costs at the level of tens of dollars for the reusable electronics part of the device, and a few dollars for a disposable patch, adding that at present, the smart bandage can be used for one to two weeks.
Gao said it is hoped the smart bandages could be used in clinics in the next five to 10 years.